|
Board Confirms Removals from the Register
At its meeting on Wednesday, 18 February, the Board of NMBI confirmed the names of those who are removed from the Register of Nurses and Midwives for failure to renew their annual registration.

At its meeting on Wednesday, 18 February, the Board of NMBI confirmed the names of those who are removed from the Register of Nurses and Midwives for failure to renew their annual registration.
The Board considers removals under Section Section77(1) of the Nurses and Midwives Act 2011, as amended. Removal notices are being issued to those who did not renew their registration for 2026. Please note that notifications of removals are sent to known employers and the Health Service Executive (under Section 82 of the Act).
All nurses and midwives who practise in Ireland must, by law, be listed on the Register of Nurses and Midwives. It is an offence to practise nursing or midwifery if your name is not on the Register. Practice includes clinical practice, nursing or midwifery management, education and research.
It is the registrant’s responsibility to ensure that their name is on the Register if they practise nursing or midwifery in Ireland.
Registrants wishing to restore their name to the Register are required to pay a restoration fee of €250 in addition to the annual registration renewal fee of €100. They must also comply with the restoration requirements at the time of application.
Spotlight On: Former President, Dr Louise Kavanagh McBride
As the 'final curtain falls' on my NMBI tenure as Board member, Vice President and President, I am very grateful and honoured for the trust, privilege, and support over the past decade.

As the 'final curtain falls' on my NMBI tenure as Board member, Vice President and President, I am very grateful and honoured for the trust, privilege, and support over the past decade.
I would like to extend my sincere gratitude to past and present NMBI Board members, senior executive team, staff, and most importantly, all our nursing and midwifery registrants. A special acknowledgement to our new President, Áine Lynch, the Chief Nursing Officer, Rachel Kenna and CEO Carolyn Donohoe, as well as former NMBI President Essene Cassidy and CEO Sheila McClelland. It’s been an absolute privilege working in collaboration with so many nurses, midwives and colleagues nationally and internally.
My time on the Board has afforded many opportunities to work in a spirit of partnership regionally, nationally and internationally. I am proud of what we have achieved for nurses and midwives, and the wider healthcare sector during my 10 years on the Board. Whilst there have been many key milestones including strategic implementations, it is important to acknowledge the evolution of the professions, key stakeholders and the Board's role in all achievements including overcoming challenges.
Three standout milestones include the national and regional roadshow events including the NMBI Series; the launch of the Code of Professional Conduct and Ethics for Registered Nurses and Registered Midwives in 2025 and the revised Nursing and Midwifery Registration Programmes Standards published in 2025. The latter two key documents will enhance guidance for nurses and midwives in Ireland and contribute to the reform of our undergraduate nurse and midwifery education programmes for the future. NMBI’s new Strategic Vision 2026 to 2029 will guide our professions, key stakeholders and the Board, with a focused strategic plan with new objectives, including the importance of NMBI’s professional support for nurses and midwives through the Compassion Project.
My initial involvement with the Board as a public appointed post in 2014 has progressed with a decade of service as a Ministerial elected Board member, Vice President and President. I would strongly encourage nurses and midwives to consider future involvement with the NMBI Board. It has been a remarkable trajectory, and I highlight how the Board must continue to transition with the importance of registrants as Board members, bringing a wealth of their knowledge and expertise to Board decision making and governance.
An extended welcome to all new Board members over the past few years, their value of engagement and contribution should not be underestimated. I would again urge nurses and midwives to participate at all levels including Board, committees and as experts.
Finally, to Áine Lynch as our new President, best wishes, continued success and fulfilment as she 'takes up the baton' in this truly privileged role. Under Áine’s stewardship, NMBI and the Board will remain committed to protecting the public and enhancing and supporting our professions in 2026 and beyond. The Nursing and Midwifery Board of Ireland is in very safe hands.
|
|
Annual State of Complaints 2024 Report Published
We have published our second annual State of Complaints report.
We have published our second annual State of Complaints report.
The 2024 report provides an overview of the fitness to practise process and covers the period from 1 January to 31 December 2024. Now in its second year, the report includes comparison data for some key information and an expanded review of the nature of the complaints received by NMBI.
As of 31 December 2024, there were 93,043 nurses and midwives registered with NMBI. Of these, 86,948 self-declared that they are practising in the professions.
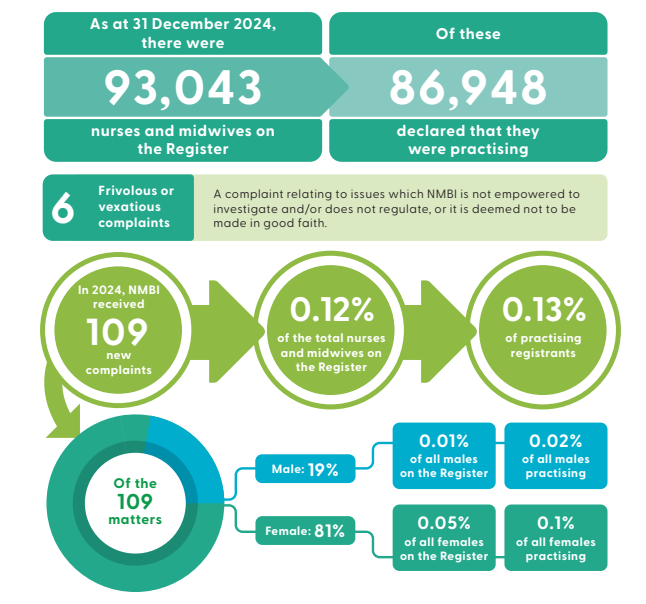
In 2024, NMBI received 109 complaints about the fitness to practise of a registered nurse or midwife which represents 0.12% of the total number of nurses and midwives on the Register. This compares to 75 complaints in 2023 (an increase of 45%) and 0.09% of the total nurses and midwives on the Register.
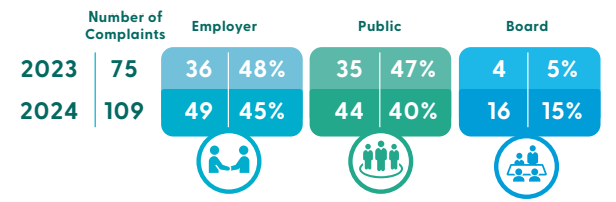
Of the 109 complaints, 49 (down 3%) were received from employers, 44 (down 7%) from members of the public and 16 (up 10%) from the Board of NMBI.
In 2024, the Preliminary Proceedings Committee (PPC) made decisions in relation to 100 complaints. 55 matters were dealt with by undertakings and/or consents and non-prima facie cases at the PPC stage (up 41% on 2023). This represents 0.06% of the total number of nurses and midwives on the Register. 45 matters were referred to the Fitness to Practice Committee (FTPC) for inquiry.

In 2024, 30 inquiries were held by NMBI (down 25%). Of these inquiries, 17% of the registrants were male (down 3%) and 83% were female (up 3%).

Eight sanctions were imposed by the Board in addition to the undertakings in the period covered in the report. This compares to 17 in 2023.
NMBI Chief Executive, Carolyn Donohoe, commented on the report, stating, “This publication offers a clear statistical view of the complaints received by NMBI against nurses and midwives and provides enhanced data into trends in our complaints process. It emphasises our unwavering dedication to robust, independent handling of complaints, prioritising public protection while supporting safe practice among registrants.”
The report is now available on our website.
Focus on Innovation and Midwifery in New Episodes of NMBI Voice
The latest episodes of our podcast, NMBI Voice are out now.
The latest episodes of our podcast, NMBI Voice are out now.
In February’s episode, Kathyann Barrett is joined by two great innovators: Una Rogers, National Nursing and Midwifery Innovation Fellow, and Anna Marie Kiernan, Registered Advanced Nurse Practitioner in Pain Medicine and National Nursing and Midwifery Innovation Fellow.
They discuss how nurses and midwives are uniquely positioned to drive meaningful change in service delivery, patient experience and operational efficiency. They highlight their successful projects using virtual reality for pain management and digital apps for crucial communication and offer practical advice on how to turn ideas into funded, successful reality.
In January, our podcast focused on the profession of midwifery. Kathyann spoke with Dr Karn Cliffe, our Director of Professional Standards - Midwifery and Lauren Walsh, a second-year midwifery student at University College Dublin and NMBI Midwifery Student Ambassador.
They discuss the role of regulation in protecting the public by actively supporting the professional development of registrants. The episode explores the unique identity of the midwifery profession, examining its core principles of art and science and its evolution towards integrated community care. It offers perspectives on education, the future of practice and the profound, privileged role of the midwife.
Listen now on Apple, Spotify or wherever you get your podcasts.
NMBI Holds Leadership Event for Senior Nurses and Midwives
On 25 February, we held a leadership event for senior nurses and midwives to enhance their knowledge and understanding of NMBI's role and the fitness to practise (FTP) process.

On 25 February, we held a leadership event for senior nurses and midwives.
The aim of the event was to enhance their knowledge and understanding of NMBI's role and the fitness to practise (FTP) process.
Attendees heard from our CEO, Carolyn Donohoe who highlighted how the NMBI is striving to make the FTP process less daunting.
Mary Devane and Emer McCormack from our Education, Policy and Standards Department, described how the Code of Professional Conduct and Ethics and the Professional Competence Scheme will support registrants to maintain the integrity of their practice.
Interim Director of Fitness to Practise, Yvanne Kennedy and Niamh McDonald, Liaison Officer provided data on the complaints made and referred to the emotional support service, while Jeanne Tarrant, Fitness to Practise Officer and Christine Hughes, Professional Advisor drew upon a real life case to illustrate the process and the possible outcomes.
We would like to thank everyone who attended and our speakers who shared their valuable insights.
Decisions Following Fitness to Practise Inquiries
The Board of NMBI has published the outcomes of three complaints following the fitness to practise process. The findings are published on NMBI's Findings and Decisions page.
The Board of NMBI has published the outcomes of three complaints following the fitness to practise process.
The findings are published on NMBI's Findings and Decisions page.
|
|
Survey Open for Registered Nurse and Midwife Prescribers on Schedule 8 Controlled Drugs
NMBI, in collaboration with the HSE Office of the Nursing and Midwifery Services Director (ONMSD), is asking Registered Nurse and Midwife Prescribers to share their views regarding prescribing of Schedule 8 Controlled Drugs in Ireland.
NMBI, in collaboration with the HSE Office of the Nursing and Midwifery Services Director (ONMSD), is asking Registered Nurse and Midwife Prescribers to share their views regarding prescribing of Schedule 8 Controlled Drugs in Ireland.
The purpose of this survey is to gain an understanding of Registered Nurse and Midwife Prescribers’ experience regarding their authority to prescribe Schedule 8 Controlled Drugs in Ireland (Misuse of Drugs Regulations, 2017, amended 2024).
If you are a Registered Nurse or Midwife Prescriber, we would encourage you to share views and experiences. Your insight is critical and will be used to inform future policy direction and professional regulation.
The survey takes approximately 10 minutes to complete and is confidential and anonymous. To take part, scan QR code below or visit the HSE website.
The survey closes on Friday, 27 February 2026.

Update: Implementation of Recommendations 24 and 25 of the ERB on Nursing and Midwifery
The Report of the Expert Review Body (ERB) on Nursing and Midwifery, published in March 2022, set out 47 recommendations aimed at strengthening and developing the professions in line with population health priorities and patient care needs.

The Report of the Expert Review Body (ERB) on Nursing and Midwifery, published in March 2022, set out 47 recommendations aimed at strengthening and developing the professions in line with population health priorities and patient care needs. The recommendations focus on workforce planning, education and professional development, digital health, and governance and leadership.
To advance this work, five Implementation Action Groups (IAGs) were established in 2023 to oversee and deliver the recommendations.
Focus on Recommendations 24 and 25
Recommendations 24 and 25 focus on developing a national clinical academic career framework for nursing and midwifery, creating stronger links between clinical practice, academic research, education and professional development.
Together, these recommendations aim to co-develop a structured clinical academic career framework and clear pathways for implementation, including the establishment and sustainability of joint clinical-academic appointments within the nursing and midwifery professions. These roles are typically co-funded by healthcare organisations and third-level institutions and support research initiatives that is directly relevant to population and service needs.
The framework will support nurses and midwives to work in both clinical practice and academia, leading and supporting research that improves nursing and midwifery care. Joint clinical academic post holders can establish themselves as both academics and practicing clinicians whilst facilitating relevant research within their clinical disciplines and extending the knowledge base for evidence informed nursing or midwifery.
- Recommendation 24: The HSE, in partnership with Higher Education Institutions (HEIs) and the Health Research Board (HRB), to develop a nationally agreed clinical academic career framework* for nurses and midwives.
*A formal clinical academic career framework allows nurses and midwives to continue in a clinical role while at the same time undertaking research to improve patient outcomes.
- Recommendation 25: The Office of the Nursing and Midwifery Services Director (ONMSD), with the Higher Education Institutions, to further develop joint nursing and midwifery clinical-academic appointments across acute and community settings.
Governance and Work Streams
To support implementation, a national project group was established and is co-chaired by an Area Director within the ONMSD and a Professor of Nursing from a higher education institution. Membership of the group reflects broad national representation and includes a Health Region Director of Nursing and Midwifery; the Technological Higher Education Association; the Irish Universities Association; Ph.D. students; midwifery and all disciplines of nursing; the Nursing and Midwifery Planning and Development Units; the National Clinical Leadership Centre for Nursing and Midwifery; the HSE Academic and Research Office; the HSE library; the Irish Research Nurses and Midwives Network; the Healthcare Research Board; the HSE/HRB funded Patient Safety Research Network; the Department of Health Chief Nursing Office; the Department of Further and Higher Education, Research, Innovation and Science; the Health Research Charities of Ireland and the NMBI.
Four dedicated work streams are supporting the delivery of the recommendations. These include:
- Work Stream 1: Two systematic literature reviews on international evidence
- Work Stream 2: Design and development of the clinical academic career framework
- Work Stream 3: Development of sustainable implementation pathways
- Work Stream 4: Advice on the number and type of clinical academic roles required nationally.
Progress to date and how to get involved
Significant progress has already been achieved. Two systematic literature reviews have been completed, with their protocols submitted for publication.
In addition, two national surveys are currently underway. One survey aims to establish the number and type of joint clinical academic nursing and midwifery appointments across Ireland. The second survey seeks information from nurses and midwives who are currently undertaking, have completed, or have started a Ph.D or professional doctorate.
Nurses and midwives who meet these criteria and who are living or working in Ireland are encouraged to participate. Their input will help build a comprehensive picture of the clinical academic nursing and midwifery workforce and will inform future planning and implementation of clinical academic career pathways nationwide.
If you are interested in completing this survey, please click here or scan the QR code below to access the survey.

In late spring 2026, once a draft of the Clinical Academic Career Framework has been developed, the project team will invite nurses and midwives to share their views on its relevance and suitability for the Irish context.
Share this news with your colleagues and if you have any queries or are interested in hearing more about this work or the development and implementation of the clinical academic career framework, you can email: erb24and25@hse.ie
|
|
Meet Our Student Ambassador: John Mc Quaid, Third-year Mental Health Nursing Student at Dundalk Institute of Technology
In this issue we speak with John Mc Quaid, a Mental Health Nursing student whose passion for the profession was developed through learning about its wide range of specialties and its potential to create meaningful change. For him, mental health nursing aligned with his values of compassion, growth and improving lives. Through his studies and leadership roles as a Class Representative and as our Student Ambassador, he has witnessed the power of connection, empathy and teamwork.
We are delighted that he has partnered with us as a student ambassador and we believe his passion and commitment will be great for the profession.

Hello, my name’s John and I’m currently a Mental health nursing student at Dundalk Institute of Technology.
I honestly never planned to study mental health nursing but when I heard stories of the opportunities it offered; the research, the endless specialties, it was my first choice on the CAO.
Before commencing my training, I asked myself what three things would you like your career to be defined by. For me, I wanted a dynamic environment, a chance to be involved in change and the privilege to improve as many people’s lives as possible. Mental health nursing has offered all of this and more.
 When I entered the Dundalk IT nursing building for the first time, I questioned my decision. It felt like I was a world apart from my friends who all shared a different building to me. I wondered if I had made a mistake, maybe I should’ve played it safe and followed my friend group, safety in numbers and all that. What I can say is that after day one, that notion vanished. I was hooked. Every word spoken, every slide presented and every booklet I read confirmed that a year prior, 17-year-old me had made the right call. When I entered the Dundalk IT nursing building for the first time, I questioned my decision. It felt like I was a world apart from my friends who all shared a different building to me. I wondered if I had made a mistake, maybe I should’ve played it safe and followed my friend group, safety in numbers and all that. What I can say is that after day one, that notion vanished. I was hooked. Every word spoken, every slide presented and every booklet I read confirmed that a year prior, 17-year-old me had made the right call.
Over the past three years, I have spent countless hours learning, engaging and developing my practice with the help of staff, students and all the service users I’ve had the privilege to interact with. These moments have shaped who I am as a nursing student, resulting in a deep passion for all things mental health and recovery.
Each module I’ve completed has covered a diverse range of topics which have been taught with the student in mind. We all learn differently, mental health nursing utilises a mixed approach to teaching in the hopes that every student’s unique strengths are supported. I find that this course offers numerous opportunities for self-expression and gives students a platform to relate their personal interests to positive mental health.
Since the first year, I have been lucky enough to assist with open days, lectures, trainings, presentations and induction days. These moments have shown me the impact student nurses can have on others and that although we are in training, we still have valuable insight to offer. My college education and practical training have shown me time and time again the power that conversation and connection hold. How simply listening can a change a person’s perspective. How offering support can alter the path they decide to take. And how showing just an ounce of compassion, can improve their life immensely.
 Of course, with any degree, there are ups and downs. We often doubt our ability, worry about mistakes we have yet to make and fear that eventually we will be left behind. Mental health nursing challenges this thinking pattern. It fosters a safe learning environment in which the class becomes a team immediately. We are not alone on our nursing journey and we share the same struggles and low moments, but by supporting each other we find the path that is right for us. This sentiment is what makes me proud to be a mental health nursing student, Class Representative and NMBI Student Ambassador. With the current growth of mental health and recovery in Ireland, I hope to see an increase in the number of nursing professionals across the nation. Of course, with any degree, there are ups and downs. We often doubt our ability, worry about mistakes we have yet to make and fear that eventually we will be left behind. Mental health nursing challenges this thinking pattern. It fosters a safe learning environment in which the class becomes a team immediately. We are not alone on our nursing journey and we share the same struggles and low moments, but by supporting each other we find the path that is right for us. This sentiment is what makes me proud to be a mental health nursing student, Class Representative and NMBI Student Ambassador. With the current growth of mental health and recovery in Ireland, I hope to see an increase in the number of nursing professionals across the nation.
I’d like to thank my lecturers for granting me the opportunity to represent my classmates with NMBI and hopefully encourage people from all backgrounds to pursue nursing as a career. I owe them a great deal for encouraging my growth as a student nurse and future healthcare professional, as they push me to expand my knowledge and remain open to change.
I want to also thank my classmates for supporting me during our training and embodying what it means to be a mental health professional. Finally, I wish to thank my fellow ambassador and good friend Modesta for joining me and offering constant guidance and support during my training.
|
|
|